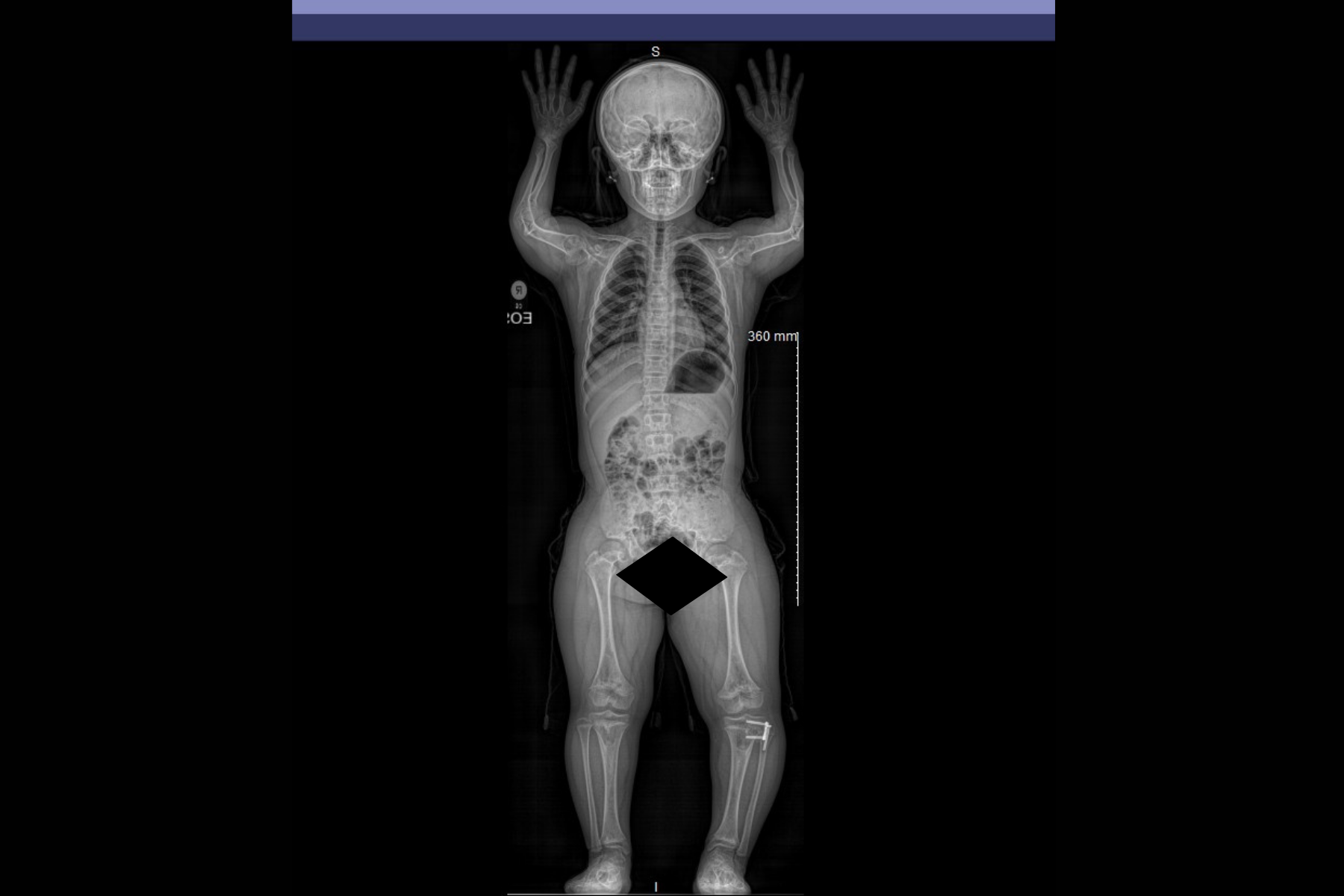
Understanding the Achondroplasia Spine
Achondroplasia is the most common form of skeletal dysplasia, caused by a genetic change in
the FGFR3 gene that affects bone growth. While children with achondroplasia have average
intelligence and life expectancy, their bone shape and growth pattern are different; particularly
in the spine.
The spine in achondroplasia is characterized by a shortened pedicle structure, decreased canal
diameter, and increased thoracolumbar kyphosis and lumbar lordosis. These features make
the spinal canal narrower and can lead to crowding of the spinal cord and nerve roots, especially
in the lower back (lumbar region).
Although not every child develops symptoms early, understanding the unique spine anatomy of
achondroplasia is essential to prevent complications, guide growth, and ensure children maintain
mobility and independence throughout development.
Common Spine Problems in Children with Achondroplasia
Children with achondroplasia are prone to several distinct spinal issues that evolve as they grow:
1. Thoracolumbar Kyphosis:
A forward curvature at the junction between the thoracic and lumbar spine often appears
in infancy. In most infants, this resolves with sitting balance and muscle strength, but in
others, it can become rigid and lead to progressive deformity.
2. Foramen Magnum Stenosis (Cervicomedullary Compression):
The opening at the base of the skull can be too small, compressing the brainstem and
upper spinal cord. This is a serious and potentially life-threatening condition that must
be screened for early in life.
3. Lumbar Spinal Stenosis:
As children grow, narrowing of the spinal canal in the lower back can compress nerves,
leading to leg pain, weakness, fatigue, or gait changes.
4. Scoliosis or Lordosis Changes:
Some children develop compensatory curvature or exaggerated lumbar lordosis that may
need close monitoring.
Diagnosis and Evaluation:
At the Paley Orthopedic & Spine Institute, children with achondroplasia undergo a detailed and
thoughtful evaluation that includes:
- Physical and Neurologic Exam: Assessing tone, reflexes, gait, and signs of cord
compression. - Imaging Studies:
* EOS imaging for low-dose full-body alignment evaluation.
* MRI of the spine and foramen magnum to assess the spinal canal, cord, and
nerve roots.
* CT scans when detailed bony anatomy is required for surgical planning. - Sleep studies or neurophysiologic tests when there are symptoms of central or
obstructive sleep apnea, which may indicate upper spinal compression.
This multidisciplinary approach ensures that decisions about timing and type of treatment are
based on a comprehensive view of both the skeletal and neurologic systems.
Treatment Options
Observation and Bracing
Many infants and young children are managed non-surgically. Flexible kyphosis can often be
corrected through positioning, physical therapy, and bracing that encourages proper posture as
trunk control improves.
Surgical Intervention
Surgery becomes necessary when deformities are rigid, progressive, or associated with
neurologic compromise. The type of surgery depends on the spinal region involved:
- Foramen Magnum Decompression:
In infants with brainstem compression, careful decompression relieves pressure while
preserving stability. This is a delicate, lifesaving procedure requiring precise
neuromonitoring. - Thoracolumbar Kyphosis Correction:
For children with fixed deformity, surgery may include posterior decompression,
osteotomies (controlled bone cuts), and spinal fusion to restore alignment and stability. - Lumbar Decompression for Stenosis:
In older children, removal of bone from the spinal canal (laminectomy or laminoplasty)
can relieve nerve compression and restore walking endurance and function.
Whenever possible, I employ growth-preserving techniques, maintaining motion
and avoiding unnecessary fusion at a young age.
My Approach to Achondroplasia Spine Care
I combine cutting-edge surgical technology with deep experience in pediatric spinal deformity and skeletal dysplasia. My philosophy is centered on three principles:
- Preserve Growth: Operate only when necessary and protect open growth plates and
motion segments whenever possible. - Maximize Safety: Use intraoperative navigation, 3D imaging (O-arm), and
neuromonitoring to achieve precise, controlled correction with minimal risk. - Individualize Care: No two children with achondroplasia are alike. Surgical plans are
customized based on the child’s anatomy, symptoms, and long-term functional goals.
Working within the Paley Orthopedic & Spine Institute, I collaborate with
world-renowned colleagues and a multidisciplinary team; including neurosurgery,
rehabilitation, and genetics, to ensure comprehensive, long-term care.
What Families Should Know
- Early screening is essential. MRI of the foramen magnum and spine is recommended in
infancy and early childhood to catch problems before symptoms appear. - Watch for signs of nerve compression: difficulty walking long distances, changes in
gait, weakness, numbness, or sleep disturbances. - Avoid unsupported sitting in young infants until trunk control develops to reduce
progression of thoracolumbar kyphosis. - Plan for multidisciplinary care: children with achondroplasia benefit from coordinated
orthopedic, neurologic, and rehabilitative support.
Families should know that with modern surgical planning, precise technology, and long-term
follow-up, children with achondroplasia can grow, walk, and thrive with an excellent
quality of life.
Looking Ahead
Spine care in achondroplasia has advanced dramatically over the past decade. Surgeons now
have access to 3D navigation, modular implants, and growth-friendly strategies that allow for
correction without compromising motion or height potential.
I, Dr. Hariharan, and the Paley team continue to lead international efforts in improving outcomes
and defining best practices for skeletal dysplasia care. For families, this means earlier diagnosis,
safer surgery, and more predictable recovery.
Consultation and Contact
If your child has achondroplasia or spinal symptoms related to dwarfism, you can learn more or
schedule a consultation with Dr. Arun Hariharan at the Paley Orthopedic & Spine Institute in
West Palm Beach, Florida.