When a parent hears the word ‘scoliosis’, they often picture a single condition with a
single treatment plan. In reality, scoliosis is an umbrella term for several distinct
diagnoses that differ in cause, timing, behavior, and management. Understanding what
type of scoliosis your child has is the first step toward getting the right care.
What All Scoliosis Has in Common
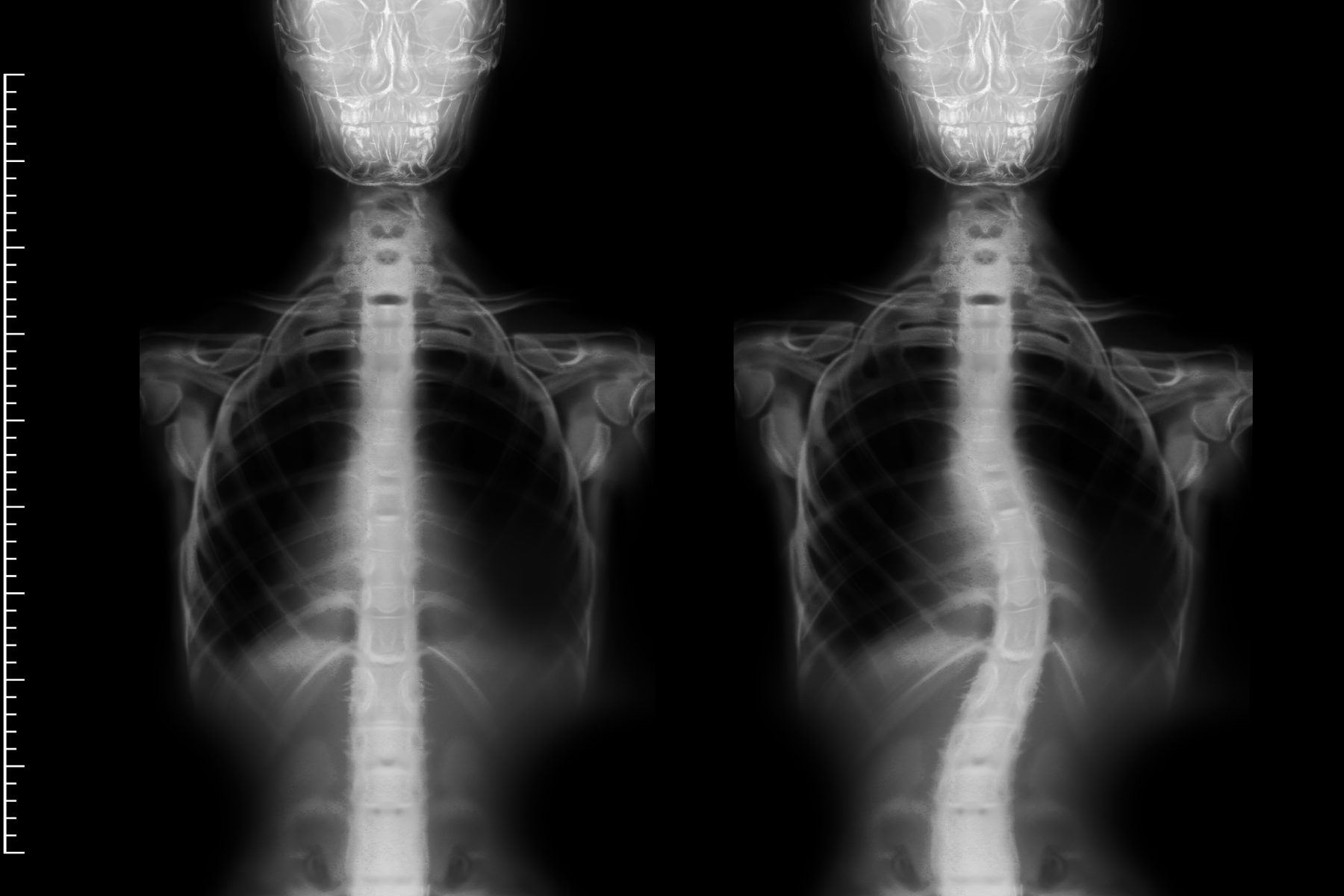
Every form of scoliosis involves an abnormal lateral curvature of the spine greater than
10 degrees, typically accompanied by vertebral rotation. That rotation, the three-
dimensional twisting of the spine, is what distinguishes scoliosis from simple postural
asymmetry and what makes it visible on a forward-bend test as a rib hump or flank
prominence.
Beyond that shared definition, the causes, progression patterns, and treatment
strategies diverge significantly.
Idiopathic Scoliosis: The Most Common Type
Idiopathic scoliosis, meaning no single identifiable cause, accounts for
approximately 80% of all scoliosis cases. It is further categorized by age at diagnosis:
- Infantile idiopathic scoliosis (birth to age 3) — Rare. Curves may resolve
spontaneously in some cases, but others progress aggressively and require early
growth-friendly intervention. - Juvenile idiopathic scoliosis (ages 3–9) — Has the highest risk of progression
among the idiopathic types. Children in this age group have significant growth
remaining, meaning a small curve today can become a large curve by
adolescence. Close surveillance and early bracing are often indicated. - Adolescent idiopathic scoliosis (ages 10–18) — The most common form of
pediatric scoliosis, affecting roughly 2–3% of the adolescent population and
disproportionately affecting girls. Curves typically worsen during growth spurts
and stabilize around skeletal maturity.
Genetics plays a role, approximately 30% of adolescent idiopathic scoliosis patients
have a family history, but no single gene explains the condition. Current research
points to a multifactorial origin involving growth plate asymmetry, vertebral morphology,
and postural control.
Congenital Scoliosis
Congenital scoliosis arises from a failure of normal vertebral formation during fetal
development, typically in the first six weeks of gestation. The vertebrae may be
malformed (hemivertebrae – wedge-shaped bones that cause asymmetric growth), fail
to separate (unsegmented bars – two vertebrae fused together, causing one side of
the spine to grow faster than the other), or a combination of both.
Because the structural problem is bony rather than soft-tissue, congenital scoliosis
tends to behave differently than idiopathic scoliosis:
- The natural history is less predictable — some curves remain stable, others
progress relentlessly - Progression depends heavily on the type and location of the anomaly
- Associated anomalies of the kidneys, heart, and spinal cord are common and
require systematic evaluation at diagnosis - Surgery is more often required and at younger ages, sometimes in infancy
Early referral to a specialist in congenital spinal deformity is critical. Treatment decisions
in this population require detailed imaging, including MRI to evaluate the spinal cord,
and a thorough understanding of the specific vertebral anatomy.
Neuromuscular Scoliosis
Neuromuscular scoliosis develops as a consequence of an underlying neurological or
muscular condition that compromises trunk muscle function and postural control.
Common underlying diagnoses include:
- Cerebral palsy (CP) — the most common cause of neuromuscular scoliosis
- Spinal muscular atrophy (SMA)
- Muscular dystrophy (Duchenne and others)
- Myelomeningocele / spina bifida
- Spinal cord injury
- Arthrogryposis multiplex congenita (AMC)
Neuromuscular scoliosis tends to be more severe, affects larger portions of the spine
(often including the pelvis), and progresses more aggressively than idiopathic scoliosis,
frequently continuing even after skeletal maturity. Curves in this population often
exceed 50–60 degrees and are associated with significant functional decline: difficulty
sitting, increased caregiver burden, respiratory compromise, and pain.
Bracing is generally less effective in neuromuscular scoliosis but may be used to slow
progression, improve sitting balance, and delay surgery in younger patients. Surgical
correction, typically involving long fusion constructs extending to the pelvis, is often
required and should be timed carefully relative to the patient's pulmonary status and
overall medical condition.
Syndromic Scoliosis
A fourth category worth understanding is syndromic scoliosis, curves occurring in the
context of specific genetic syndromes such as Marfan syndrome, Ehlers-Danlos
syndrome, Prader-Willi syndrome (PWS), Rett syndrome, or neurofibromatosis. These
cases often combine features of idiopathic and neuromuscular scoliosis and may
require specialized management specific to the syndrome.
Why the Type Matters
The type of scoliosis your child has directly determines the recommended surveillance
interval, the likelihood of curve progression, the appropriateness of bracing, the timing
and type of surgery (if needed), and the long-term prognosis.
This is not a condition where one-size-fits-all management applies. A 25-degree curve
in a healthy 13-year-old girl with idiopathic scoliosis is managed very differently from a
25-degree curve in a 6-year-old with SMA or a 25-degree congenital curve from a
hemivertebra.
The Bottom Line
Getting the diagnosis right, including the specific type of scoliosis, is the foundation
of a successful treatment plan. If your child has been told they have scoliosis, asking
your provider which type they have, what the natural history is for that specific type, and
what the monitoring and treatment plan looks like are entirely appropriate questions. A
subspecialty-trained pediatric spine surgeon can provide a complete evaluation and
guide your family through the nuances that matter most.
Dr. Arun Ramaswamy Hariharan is a pediatric spine surgeon at the Paley Institute at St. Mary’s
Medical Center in West Palm Beach, FL, specializing in adolescent idiopathic scoliosis, early
onset scoliosis, and complex spinal deformity. To schedule a consultation, visit
scolisurgeon.com.